IUD Insertion and Removal
An intrauterine device (IUD) is most commonly known as a form of long-acting, reversible birth control. However, the applications of IUDs extend further than contraception, including effective management of several common life-impacting gynaecological conditions.
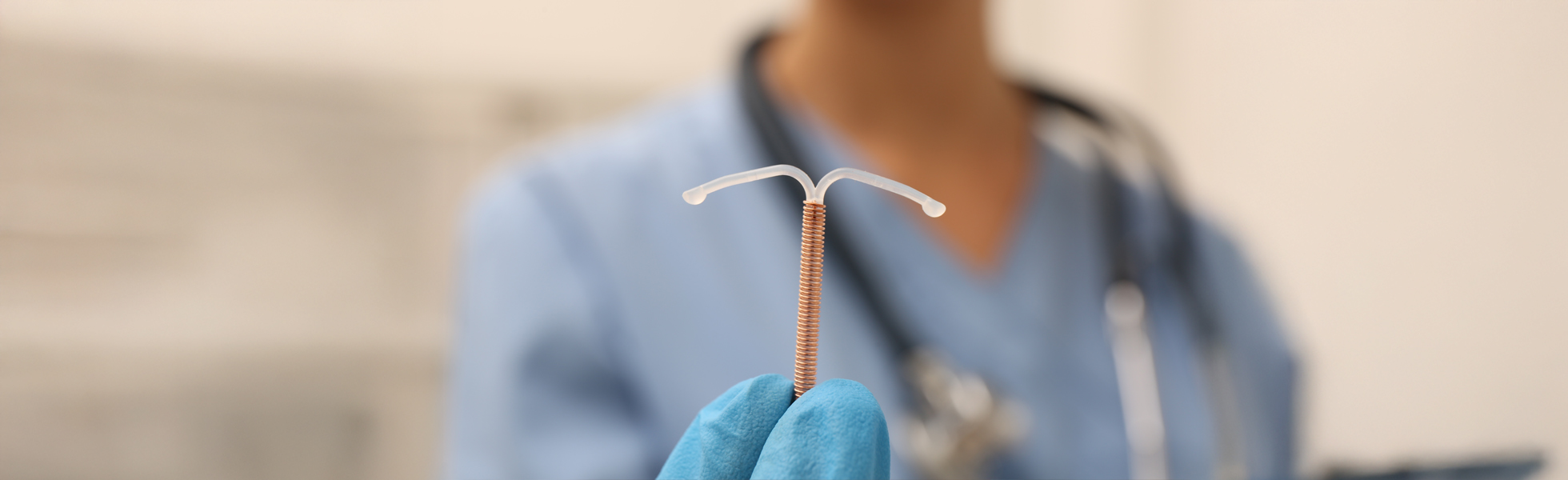
How does an IUD work?
An IUD is a T-shaped device that is inserted into your uterus via the cervix, and is a highly effective method of preventing pregnancy.
There are currently two types of IUDs available in Australia. A hormonal IUD works by slowly releasing a hormone that interferes with sperm reaching and fertilising your egg, shortening the lifespan and availability of the egg, and thinning your uterine lining to make it more difficult for a fertilised egg to implant. This hormone, known as levonorgestrel, may also prevent ovulation in some women.
A copper IUD is a non-hormonal contraceptive device. Instead, copper ions are released from the device, which creates an environment that is toxic to both sperm and eggs, and alters your uterine lining to effectively minimise the likelihood of falling pregnant. Unlike a hormonal IUD, copper IUDs do not impact ovulation or your menstrual cycles.
Both IUDs can remain in your body for years – the hormonal IUD is currently approved for up to 8 years and the copper IUD for up to 12 years, before they require replacing.
Benefits of IUDs as contraception
As a form of birth control, IUDs are extremely effective, with a success rate of over 99% at preventing pregnancy. Compared to other types of contraception, IUDs:
- Don’t rely on you to remember to take a daily oral contraceptive pill or use a condom
- Are more cost-effective in the long-term
- Can be used while breastfeeding
- Don’t have long-term impact on your fertility once removed
When considering whether an IUD is right for you, be aware that they aren’t suitable for all women. IUDs also come with potential complications such as the device shifting position inside your uterus or coming out on its own, or the risk of infection after the device has been inserted.
Other uses for IUDs
Hormonal intrauterine devices have additional uses outside of contraception, as they have the added benefit of reducing or pausing ovulation and menstrual bleeding. Dr Sam may suggest an IUD as a treatment option if you have:
- Abnormally heavy periods
- Especially painful menstrual periods
- Endometriosis, a condition involving abnormal growth of tissue similar to the lining of your uterus
- Polycystic ovary syndrome (PCOS), a common condition characterised by irregular periods, elevated levels of male hormones, and infertility
- Uterine fibroids
Inserting an IUD can help to minimise the pain, discomfort, and inconvenience from the menstrual bleeding often associated with these common conditions.
How IUD insertion and removal works
An IUD must be fitted by an appropriately trained doctor who not only can perform the procedure but also provide the right advice for your situation, including whether you should not have an IUD.
How is an IUD inserted?
Prior to having your IUD fitted, Dr Sam will confirm there’s no pelvic infection present and that you are not currently pregnant. IUD insertion can be performed in the clinic as a short procedure.
You will be positioned on your back with your knees raised, similar to having a cervical screening test/pap smear. A local anaesthetic may be sprayed into your vagina and cervix to make the procedure more comfortable for you, and then the intrauterine device is passed through your cervix into position in your uterus. The IUD is attached to a thread that will hang into your vagina. This string can be used for you to check that the IUD is still in place, and can also be used for removing the device in the future.
After having your IUD inserted, you should avoid baths, swimming, sexual intercourse, and using tampons for a few days to reduce your risk of an infection.
How is an IUD removed?
IUD removal is typically very quick and straightforward, performed in Dr Sam’s office. Pulling gently on the IUD string slides the device out with minimal discomfort. If you are replacing it, the new one can be inserted during the same appointment.
On rare occasions, an IUD may become embedded, meaning the device has become lodged in the wall of your uterus or cervix and cannot be easily removed. Most women are entirely unaware this has happened, but some may notice symptoms such as pelvic pain, painful intercourse, or bleeding between periods. If the IUD strings cannot be found, Dr Sam can confirm an embedded IUD through ultrasound. You may then need a hysteroscopy procedure to remove the device.
IUD insertion in Sydney with Dr Sam Daniels
As a highly trained specialist focused exclusively on gynecology, Dr Sam Daniels has performed countless IUD procedures for all sorts of reasons, including for birth control and management of other gynaecological conditions. One of his specific areas of expertise is in the treatment of abnormal menstrual bleeding, positioning him well to offer symptom relief with an intrauterine device where appropriate.
Frequently Asked Questions
No, IUD insertion is not considered painful, though there may be some cramping-like discomfort when the speculum is inserted into your vagina to hold apart the walls. Dr Sam uses a local anaesthetic to minimise the sensation of pain.
A properly placed IUD shouldn’t be noticeable, even during sexual intercourse. You should be able to feel the thread attached to it if you try to find it with your fingers, but this string is also otherwise unobtrusive.
The most severe risk of an IUD is the potential for it to perforate through the uterus wall. This complication is extremely rare and most likely to happen during insertion. Other risks include a small risk of infection in the few weeks after insertion, or the possibility of an ectopic pregnancy (a fertilised egg implanting in your fallopian tubes instead of uterus) in the unlikely event of the IUD failing.
Specialist care for women’s health concerns
Comprehensive care with Dr Sam Daniels is available across multiple Sydney locations, including urgent gynaecologist appointments for time-sensitive cases.