Uterine Fibroids
Uterine fibroids are an exceedingly common gynaecological condition, affecting up to four out of five women in their lifetime. While some fibroids cause no problems, other women experience impaired quality of life through painful and uncomfortable symptoms, infertility, and recurrent miscarriages.
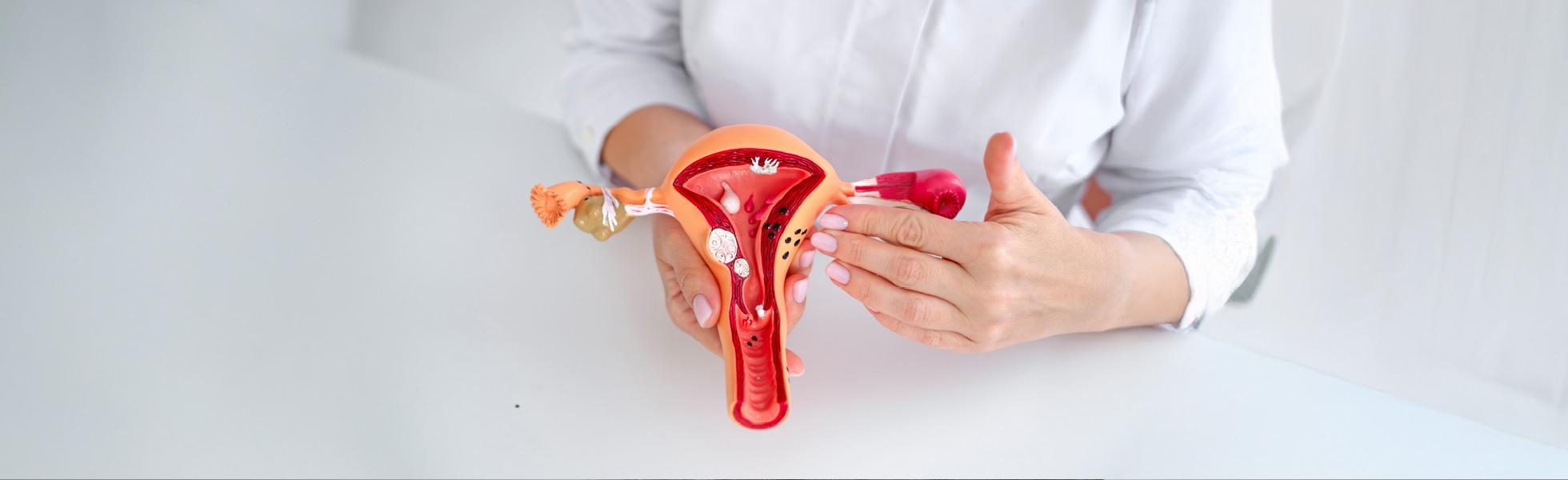
What are uterine fibroids?
Uterine fibroids are non-cancerous growths in the uterus, also known as your womb. Fibroids can be quite variable in size, and you may have more than one. There are three locations around the muscle wall of the uterus where a fibroid may develop:
- Submucosal fibroids grow on the inner surface of the uterus
- Intramural fibroids develop inside the uterine muscle tissue itself
- Subserosal fibroids form on the outer surface of the uterus
The cause of uterine fibroids is not well-understood, though doctors believe oestrogen and progesterone hormones play a role. Because of the decrease in the levels of these hormones after menopause, you may find your fibroid-related symptoms can improve once you pass menopause, and some fibroids may even resolve on their own at this stage.
Risk factors for fibroids
Certain factors can increase your risk of developing uterine fibroids, including:
- A family history of fibroids, especially a first-degree relative
- Being aged between your 30s up to menopause
- Asian ethnicity
- Being overweight or obese
- Eating a diet high in red meat and ham
Having one or all of these risk factors increases your chances of having fibroids but does not guarantee you will get them or that they will be problematic. Conversely, even if you have none of these risk factors, it is still possible to develop uterine fibroids.
Symptoms of uterine fibroids
Many women with fibroids are entirely asymptomatic, and only become aware of a uterine fibroid during a pelvic ultrasound for another reason. Depending on the location, size, and nature of a uterine fibroid, you may experience:
- Heavy or irregular menstrual periods
- Infertility and recurrent pregnancy loss
- Painful periods
- Bleeding between periods
- Pain during sexual intercourse
- The sensation of pressure around your pelvis and lower back
- Needing to urinate frequently
- Constipation
How do uterine fibroids cause infertility?
Uterine fibroids can impact your ability to fall pregnant and maintain a healthy pregnancy, mainly by interfering with successful implantation of a fertilised embryo in the lining of your uterus. Usually it is submucosal fibroids that will cause problems with fertility in this way.
Uterine fibroids are also associated with pregnancy complications, such as needing a Caesarean section, the baby being breech (positioned feet first rather than head first during delivery), pre-term delivery, or placental complications. Many women with uterine fibroids will fall pregnant with no problems and progress smoothly through their pregnancy, labour, and delivery. However, if you are experiencing difficulty conceiving, surgical treatment to remove the fibroids may improve your fertility. For women who are still experiencing infertility despite uterine fibroid surgery, Dr Sam can refer you to a fertility specialist to consider your options with assisted reproductive technologies.
Uterine fibroid treatment
A comprehensive examination with Dr Sam Daniels will guide his treatment recommendations for your situation. If you aren’t suffering from any bothersome symptoms like pain or infertility, it’s safe to monitor it at frequent intervals with imaging.
How are uterine fibroids diagnosed?
Uterine fibroids may be diagnosed through imaging such as a pelvic or vaginal ultrasound, or MRI. If the imaging scans are inconclusive or unable to provide enough detail, Dr Sam may perform a surgical procedure known as laparoscopy, where a long, thin scope is inserted through an incision in your abdomen to view your uterus. Alternatively, he can examine the inside of your uterus with hysteroscopy, another specialist procedure where the scope is inserted via your cervix. The information provided by these imaging procedures, including the size and location of the fibroids, are combined with other considerations such as your age, future family plans, and symptoms, to decide on the most suitable treatment approach.
Medical management for uterine fibroids
Some uterine fibroids can effectively be managed using non-surgical treatments. Oral medications including the oral contraceptive pill, hormone implants and injections, RyeqoⓇ, or intrauterine devices (IUDs), can either act to reduce the size of your fibroids or alleviate your symptoms. These medicines do come with a risk of side effects, such as the fibroids rapidly regrowing once you cease the therapy. Dr Sam will discuss the benefits and risks of medical therapy if he believes this is an appropriate treatment option for you. You may find that fibroid-related pain can be adequately managed with off-the-shelf pain medication, and iron supplements can be taken to treat iron-deficiency anaemia resulting from heavy periods.
Uterine fibroid surgery
Uterine fibroids causing moderate to severe symptoms are often more effectively managed through surgery. There are a few approaches to uterine fibroid surgery available with Dr Sam.
Myomectomy
A myomectomy aims to remove the fibroids without compromising your uterus, which makes it the best option for women who still want to have children in the future. As a surgeon with advanced training in minimally invasive techniques, Dr Sam usually performs myomectomy with laparoscopy or hysteroscopy. Depending on the size and location of the fibroids, however, open surgery may be necessary in certain cases. It is possible for fibroids to regrow after a myomectomy.
Hysterectomy
A hysterectomy is a surgical procedure to remove the entire uterus. This procedure guarantees a cure from uterine fibroids, but also means you can no longer carry a pregnancy. Dr Sam only recommends a hysterectomy for women who have particularly large or numerous fibroids, those with severe and heavy menstrual bleeding, or for women who are sure they don’t want to have children in the future. A hysterectomy can also be a good option for women who are approaching menopause or are already post-menopausal.
Endometrial ablation
For women with very heavy or prolonged menstrual bleeding who are unresponsive to or unsuitable for medical therapy, endometrial ablation may be considered. Endometrial ablation involves a variety of methods to remove or destroy the endometrium, the lining of the uterus. The vast majority of women who undergo endometrial ablation have greatly improved symptoms, with around half not experiencing periods at all anymore. Endometrial ablation is only suitable if you do not wish to have any children in the future.
Frequently Asked Questions
Fibroids are typically diagnosed after a thorough history with an experienced doctor, as well as a pelvic examination and specific imaging techniques such as a transvaginal pelvic ultrasound.
No, not necessarily. Some fibroids will be suitable for monitoring with no intervention, while others may be effectively treated or have the associated symptoms treated with medical therapy such as the oral contraceptive pill, an IUD, or other oral medications.
Specialist care for women’s health concerns
Comprehensive care with Dr Sam Daniels is available across multiple Sydney locations, including urgent gynaecologist appointments for time-sensitive cases.