
Dr Sam Daniels is a benign gynaecologist who provides expert care across Sydney in Women’s Health. Sam has undertaken additional training in advanced urogynaecology and minimally invasive surgery.
Pelvic organ prolapse occurs when there is a weakness in the tissue and potentially the supporting ligaments of the bladder, bowel or uterus. This weakness in the tissue often results in women noticing a bulge or new found 'lump' vaginally that may have not previously existed and may be accompanied by an array of symptoms.

Symptoms will vary from patient to patient, the most common symptoms that patients describe is a dragging sensation. Other symptoms include:

The treatment option of your pelvic organ prolapse will be largely dictated by the location and size of your prolapse as well as the nature of your symptoms.

Many pelvic organ prolapses will respond well to non surgical management and use of a vaginal pessary. This is a small silicon device that is placed in the vagina to reduce the bulge and can improve symptoms instantly providing relief to women. Pelvic floor physiotherapy is also often recommended as a first line treatment option.

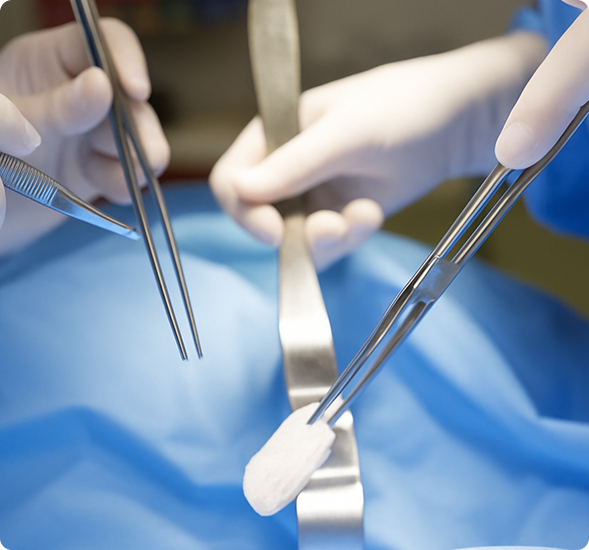
Laparoscopic or Robotic approach to repair the prolapse is very common and this is often reserved for those women whom have a global prolapse (involving the bowel, bladder and uterus). This procedure can be performed with both mesh and non-mesh alternatives. It is really important to note that it was vaginal mesh that was the focus and centre of all the media attention and class action. Dr Daniels does not perform vaginal Mesh.
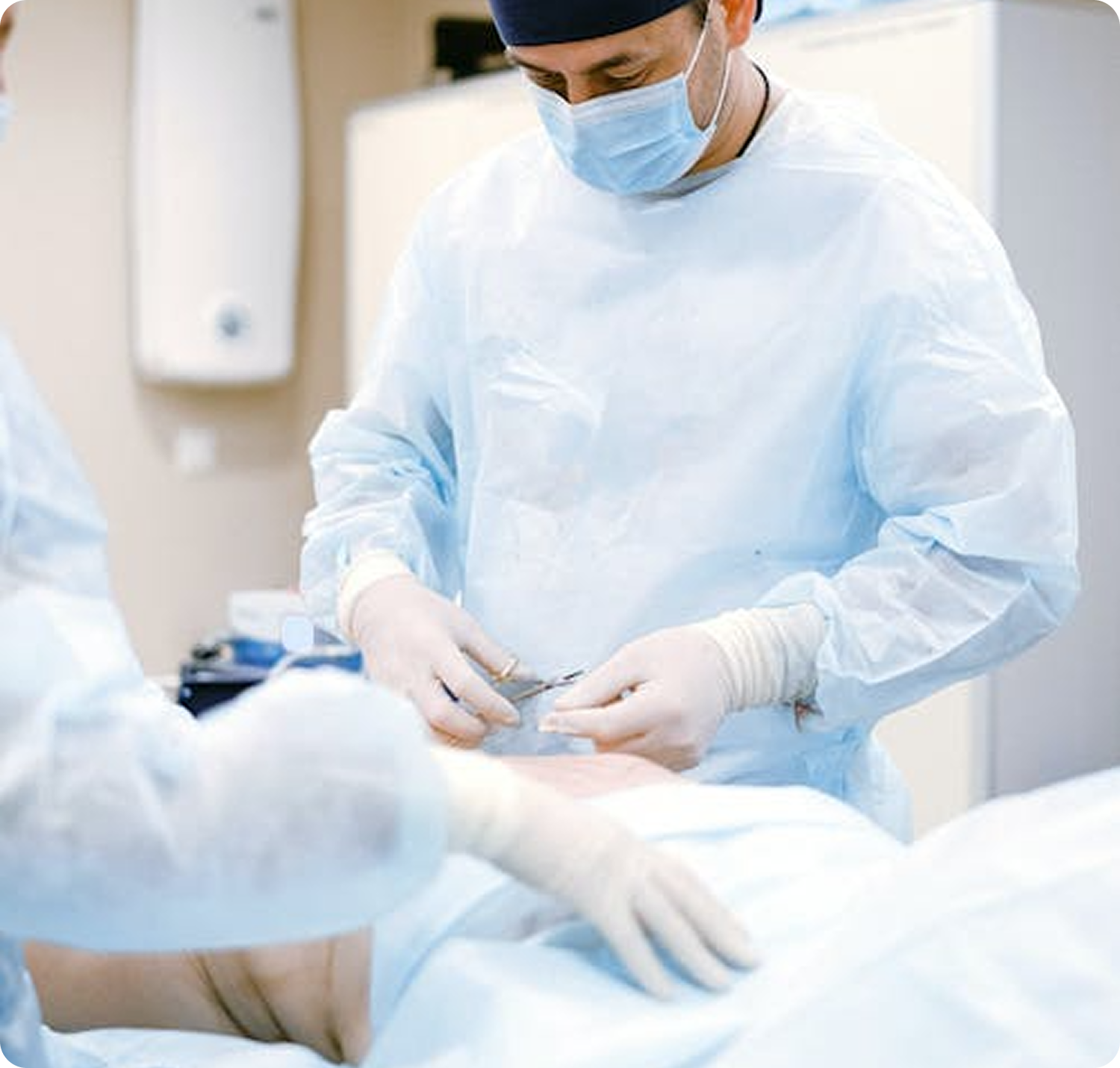
A vaginal approach is commonly used for prolapse surgery, but this is heavily dictated by the examination, patient desires and multiple lifestyle factors to consider. Vaginal approach is also considered minimally invasive with a quick recovery time.

Every patient is different and will have a unique bespoke journey for their treatment of their pelvic organ prolapse.
Patients should expect an initial 45 minute consultation that can be performed face to face of via telehealth. During the consultation:
A discussion on treatment planning will occur identifying your goals as a patient and should surgery be indicated there will be a detailed discussion about the processes, risks, costs, post-surgical management as well as time frames.
Pelvic organ prolapse occurs when there is a weakness in the tissue and potentially the supporting ligaments of the bladder, bowel or uterus. This weakness in the tissue often results in women noticing a bulge or new found 'lump' vaginally that may have not previously existed and may be accompanied by an array of symptoms.
Surgery is really only advised for those women whom continue to be symptomatic from their prolapse despite exhausting much more conservative approaches. Where appropriate, these conservative approaches may be a vaginal pessary and pelvic floor physiotherapy.
A minimally invasive approach will result in women returning to their normal duties in life much quicker due to a decreased pain requirement.
Sam is accredited to perform Laparoscopic Mesh Sacrocolpopexy and reserves this for women with significant prolapse that is affecting multiple areas or in those whom previous surgical approaches have failed to correct the prolapse.
No, It is really important to note that it was vaginal mesh that was the focus and centre of all the media attention and class action. Sam does not perform vaginal mesh surgeries and has never in his private practice.
The recovery time is highly dependent upon the nature of your surgery and its approach, but typically will require a minimum of 2 weeks off work. Sam will generally advise you to avoid sex, swimming, tampons and heavy lifting (anything greater than 7kg) for a period of 6 weeks. He will often give you advice on how to avoid constipation post the surgery to ensure that the stitches heal effectively and that there is less of a chance of recurrence of prolapse.