
Dr Sam Daniels is an endometriosis specialist in Sydney who practices excisional therapy. Sam has undertaken additional training in minimally invasive surgery and has the highest level of qualification for managing complex endometriosis cases.

Endometriosis is a condition where the tissue similar to the lining of the uterus is found in areas outside of your uterus in the pelvis, such as your ovaries, bladder or even bowel.
It affects 1 in 7 women in Australia and on average takes 6.5 years to be diagnosed with Endometriosis.
In general, endometriosis is more commonly diagnosed in women in their 20’s and 30’s, but even adolescents can be diagnosed with endometriosis.

Women can present with symptoms of endometriosis in many different ways, common symptoms include:
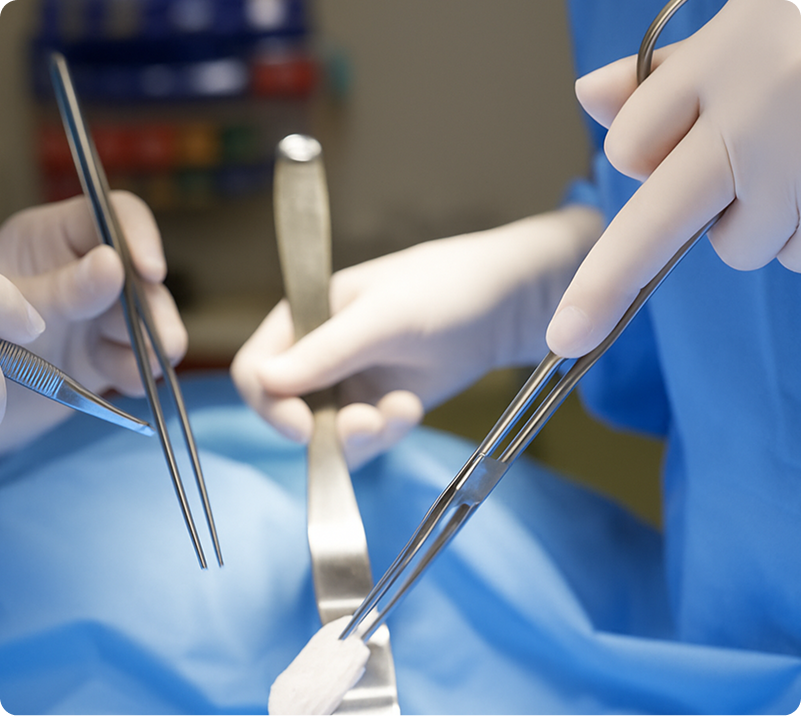

Surgical management does remain the gold standard for treatment of endometriosis. It is important that you see an endometriosis surgeon who does excisional surgery. The surgery is performed laparoscopically or robotically and is minimally invasive, allowing for a faster recovery then open surgery as well as reduced pain and a quicker return to normal duties.

Often cases can be managed initially without surgery. There is a range of medications that seek to suppress endometriosis and their symptoms. Medical management can be utilised in isolation as well as in conjunction with surgical management.

Advanced stage endometriosis affecting multiple organ sites will require collaborative care and a multi-disciplinary team may be indicated. Sam works alongside both colorectal surgeons and urologists in complex cases of deep infiltrating endometriosis, as well as other allied health professionals such as pelvic floor physio, dieticians and naturopaths to provide the latest evidence based care.

Every patient is different and will have a unique bespoke journey for their treatment of endometriosis.
Patients should expect an initial 45 minute consultation that can be performed face to face of via telehealth. During the consultation:
A discussion on treatment planning will occur identifying your goals as a patient and should surgery be indicated there will be a detailed discussion about the processes, risks, costs, post-surgical management as well as time frames.
Yes, endometriosis can recur. Best practice aims to excise endometriosis and remove the cells. If pregnancy is not desired, hormonal suppression may be recommended to try and prevent endometriosis from recurring.
Please contact Sam's reception staff to discuss his fees for surgery, the complexity of the endometriosis will dictate the fee and eligible medicare rebate.
Most patients will go home the same day of surgery, or the next day. Sam's surgeries are minimally invasive and promote prompt recovery time and early return to work.
If you think you have endometriosis! Too many women dismiss their symptoms and suffer in pain, endometriosis is a real condition, women should be heard and see by an endometriosis surgeon as soon as it is suspected.
They are specialist in management of this complex disease. They often work alongside a multi-disciplinary team to best manage your symptoms and unique situation. They will discuss management options with may be surgical excision of disease from the pelvis or medical management with medicine.
Endometriosis can be diagnosed clinically or surgically.
A clinical diagnosis is based on the symptoms of the patient and or evidence of endometriosis on examination, ultrasound or MRI.
A surgical diagnosis is made with excisional surgery of endometriosis. Where tissue is removed from the pelvis and examined under a microscope.
Guidelines have been developed that strongly suggest best practice is to excise and remove the endometriosis as opposed to ‘ablate’ or ‘burn’ the endometriosis.
Endometriosis surgery should be performed by a qualified AGES accredited laparoscopic surgeon who is accredited to perform Level 6 surgery. These surgeons have the highest level of qualification and are considered specialist endometriosis surgeons
Minimally Invasive Surgery is the best approach to excising endometriosis. It allows for a shorter hospital stay, faster recovery, earlier return to normal daily activities and reduced post operative pain. Minimally invasive surgery allows careful handling of the pelvic organ tissues, minimising risk and improving fertility outcomes, reduced pain and scarring compared to open surgery.